
Heart Disease Risk: One Diet Does Not Fit All
Vigorous Exercise for Women May Lead to Greater Health Benefits
Human Genome Lab Groundbreaking
New Device Cleans Water with Light
Research Reveals Growth Factor's Role in Cancer Treatment
New Device Lowers Radiation Exposure During Dental X-Rays
Gas Emissions Provide Clue to Volcanic Activity
New Technique Stops Spread of Hazardous Waste
Virtual Laboratories Debuting on the Internet

Research Reveals Growth Factor's Role in Cancer Treatment
Radiotherapy-the use of x-rays and other ionizing radiation to treat
cancer-involves a deadly compromise. Bombarding a tumor with cell-killing beams
inevitably affects healthy tissue in the tumor's vicinity.
Mary Helen Barcellos-Hoff, a biologist in Berkeley Lab's Life Sciences Division,
has taken an important step toward reducing complications in cancer patients
after radiotherapy. She has shown that ionizing radiation, such as that used in
cancer treatment, activates transforming growth factor-beta (TGF-
Her study provides the strongest evidence yet that the molecule is the cause of
radiogenic fibrosis, a hardening of tissue that is common following radiotherapy.
"We think TGF-
More importantly, the research suggests a new way of improving radiotherapy.
Blocking TGF-
Typically, one-fifth of cancer patients receiving radiotherapy suffer some degree
of fibrosis in the tissue surrounding a tumor. Fibrosis is the result of an
overproduction of extracellular matrix (ECM), the fibrous network of molecules
between cells that determines structure and regulates function of tissues. In
fibrosis, tissues gradually lose their elasticity as ECM fills up the space
between cells.
One of TGF-
To look at the effect of radiation on TGF-
By adding the antibodies to tissue, then using fluorescence to highlight the
antibodies, Barcellos-Hoff could look at the distribution of the two types of
TGF-
Barcellos-Hoff found restructuring of the ECM following the treatments,
suggesting that activated TGF-
Barcellos-Hoff is now examining how molecules such as antibodies could block the
effects of TGF-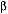 ), a
cell-signal molecule known for its role in scarring.
), a
cell-signal molecule known for its role in scarring.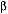 sows the seeds that determine whether or not irradiated tissue
undergoes permanent dysfunction," Barcellos-Hoff says.
sows the seeds that determine whether or not irradiated tissue
undergoes permanent dysfunction," Barcellos-Hoff says.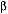 activation could decrease side effects, and provide the basis for
more aggressive radiotherapy and better tumor control.
activation could decrease side effects, and provide the basis for
more aggressive radiotherapy and better tumor control.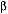 's best understood roles in the body is coordinating the production
of ECM to heal wounds. Fibrosis in some ways is like wound healing gone haywire,
with TGF-
's best understood roles in the body is coordinating the production
of ECM to heal wounds. Fibrosis in some ways is like wound healing gone haywire,
with TGF-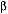 converting healthy tissue to tough tissue similar to that seen in
scars.
converting healthy tissue to tough tissue similar to that seen in
scars.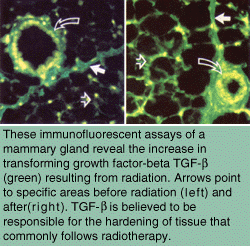 However, finding how TGF-
However, finding how TGF- might trigger fibrosis has been a challenge. The
stumbling block has been the two-faced nature of the molecule. Most growth
factors and other cell signals, such as hormones, affect surrounding tissue
immediately after release. In contrast, TGF-
might trigger fibrosis has been a challenge. The
stumbling block has been the two-faced nature of the molecule. Most growth
factors and other cell signals, such as hormones, affect surrounding tissue
immediately after release. In contrast, TGF- enters the surrounding tissue in a
latent form, bound to a larger carrier molecule known as latency-associated
peptide, and must be activated.
enters the surrounding tissue in a
latent form, bound to a larger carrier molecule known as latency-associated
peptide, and must be activated. activation, Barcellos-Hoff created an
antibody-based test that could distinguish between the two forms of the molecule.
First, she obtained genetically engineered cells, provided by collaborators at UC
San Francisco, that secreted either the latent or active form of the molecule.
She was able to grow the cells as tumor tissue, then use the tissue to select for
antibodies that would bind to one or the other form of TGF-
activation, Barcellos-Hoff created an
antibody-based test that could distinguish between the two forms of the molecule.
First, she obtained genetically engineered cells, provided by collaborators at UC
San Francisco, that secreted either the latent or active form of the molecule.
She was able to grow the cells as tumor tissue, then use the tissue to select for
antibodies that would bind to one or the other form of TGF-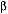 .
.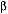 in mouse mammary tissue before and after therapy-level doses of radiation.
The tests showed that radiation had a dramatic effect on TGF-
in mouse mammary tissue before and after therapy-level doses of radiation.
The tests showed that radiation had a dramatic effect on TGF-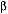 . Levels of the
latent form, which were high in the tissue to begin with, dropped sharply within
an hour of the treatment. Levels of the active form, which were nonexistent at
first, increased. Active TGF-
. Levels of the
latent form, which were high in the tissue to begin with, dropped sharply within
an hour of the treatment. Levels of the active form, which were nonexistent at
first, increased. Active TGF-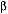 remained high for at least a week following
radiation exposure.
remained high for at least a week following
radiation exposure.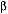 was already beginning to influence cells in the
irradiated tissue.
was already beginning to influence cells in the
irradiated tissue.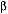 prior to radiation treatment.
prior to radiation treatment.